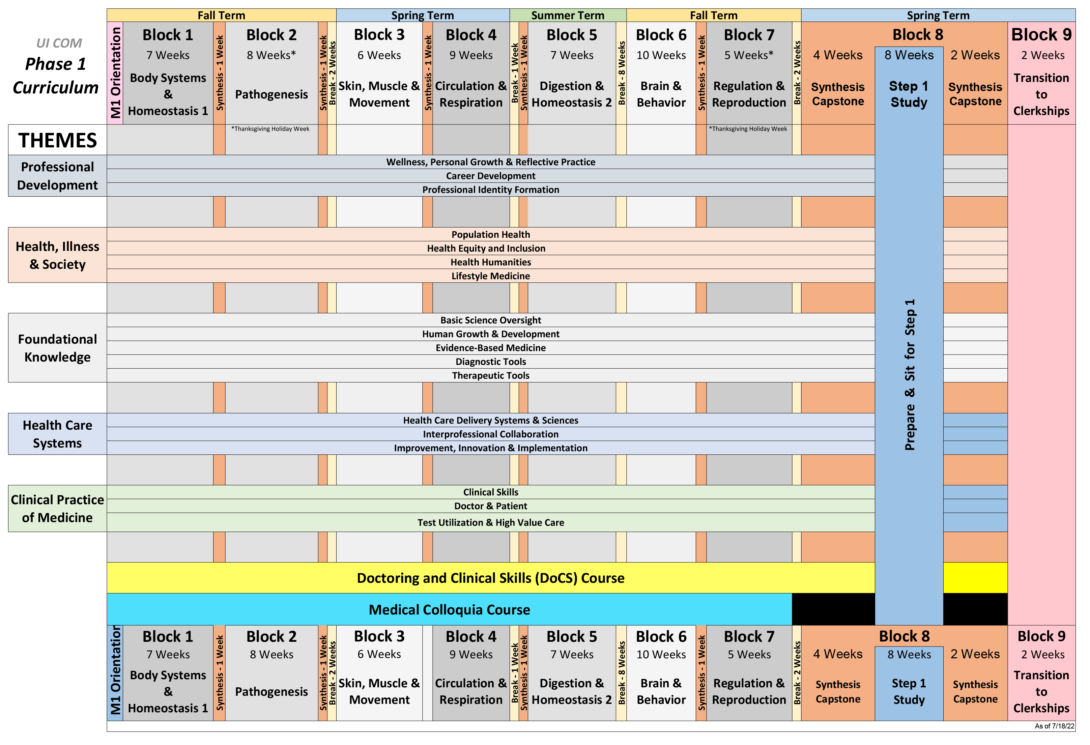
Phase 1 (Year 1 and Year 2) Curriculum
M1 & M2 Curriculum Heading link
-
Course Number: MDC 601, Credit Hours: 5
Block 1: Body Systems & Homeostasis 1 (7 Weeks) is the first introduction to the patient and healthcare system in the context of routine health maintenance and wellness. During this block, students will begin to learn about the roles and responsibilities of various members of the healthcare team. They will be introduced to the basics of the normal structure and function of the human body, including how to monitor health status using vital signs, general appearance, and laboratory tests. Students will learn the core concepts of the foundational sciences of medicine – genetics, biochemistry, immunology, microbiology, embryology, cell biology, physiology, pharmacology, evidence-based medicine – and how they relate to normal processes in the body. This core will provide the building blocks to distinguish abnormal from normal, and to understand the basis for diagnostic testing and pharmacologic interventions. They will also learn the basics of epidemiology and biostatistics to support effective clinical practice and interpretation of the scientific literature.
Doctoring and Clinical Skills (DoCS) and Medical Colloquia are also included in this block. Students will meet their first patients as a medical student, and they will practice the basics of communication and gathering history and vital signs during a patient encounter.
Students may feel overwhelmed by the large amount of material that needs to be read, digested, and integrated. That’s normal in medical school. There will be discussions on ways of maintaining personal and professional well-being, and help for developing strategies for coping with the stresses of life and school. Additionally, there will be an introduction to quality improvement processes that apply to personal and professional activities in order to become a reflective practitioner. All of the concepts introduced here will be revisited and built upon in subsequent block courses.
-
Course Number: MDC 602, Credit Hours: 6
Block 2: Pathogenesis (8 Weeks) is devoted to beginning a lifelong pursuit of understanding the etiology of disease formation and progression and the current ways to stabilize, mitigate, or even reverse the disease process using pharmacological, non-pharmacological, and complementary interventions. Students will learn about microbiology, immunology, and the tools to address infectious illness; and begin to study cancer, its origins, and its therapeutics. Alongside this, students will also learn ways to support their well-being, nurture their identity as a physician and a human, and connect with the community that they serve.
-
Course Number: MDC 603, Credit Hours: 5
Block 3: Skin, Muscle & Movement (6 weeks) begins in January following the winter break, and is the first of five block courses, extending for the calendar year through December of the M2 academic year, organized in an organ system approach. Students’ experience in the gross anatomy lab begins in this block and will extend through Block 7. This sequence is in part oriented toward the logistics of the approach to dissection (e.g., starting in this block with skin and muscular systems). The content will include study of skin, muscle and bone anatomy and physiology and include exploration of orthopedic and rheumatologic issues, physical disability, and issues in health care such as pain management and appropriate use of testing and surgical intervention in conditions such as back pain. The culmination of anatomy study is a meaningful Service of Gratitude for the gifts of the donors and their family during the M2 year.
-
Block 4:
Block 4: Circulation & Respiration (9 weeks) begins to explore fundamental physiologic and pharmacologic concepts in homeostasis, and introduces the student to some of the most common and significant health issues such as coronary disease, asthma and chronic lung disease. Many concepts in test utility, epidemiology, health systems, and health equity are also incorporated into this block.
-
Block 5: Digestion & Homeostasis 2
Block 5: Digestion & Homeostasis 2 (7 weeks) along with study of the GI and renal systems, begins to explore hormonal physiology, particularly the exocrine aspects related to GI function and endocrine issues such as diabetes and adrenal function. A number of health delivery systems and health equity issues surround the study of diabetes and of chronic kidney disease and dialysis. This block also provides many opportunities to return to the study of biochemistry and nutrition.
-
Block 6: Brain & Behavior
Block 6: Brain & Behavior (10 weeks) follows the summer break between the year 1 and year 2 academic years. Much of the peripheral nervous system would have been explored during previous blocks; here the emphasis is on the central nervous system, the special senses, and many aspects of normal and abnormal human development, psychology, and psychiatric disorders.
-
Block 7: Regulation & Reproduction
Block 7: Regulation & Reproduction (5 weeks) is the final organ system-oriented block course, and extends to the winter break of the M2 academic year. Students complete their initial study of anatomy with a focus on the pelvic floor and reproductive organs; an additional focus on endocrine function provides another opportunity to “spiral” to a deeper understanding of these complex physiologic interactions.
-
Block 8: Synthesis
Synthesis (Longitudinal) links the week-long intersessions between each block course, together with the longer, summative period of Block 8, to form a course focusing on the cumulative nature of students’ learning and the longitudinal trajectory of their professional development. In each of these course segments, students will have an interval where they are not continually responsible for “new” material but can reflect on their learning to date, consolidate and integrate their knowledge, and plan their approach to learning going forward. Class sessions will focus on cases that illustrate the interdependence of the organ systems studied to date and the management of complex, multi-system disease. The Professional Development Theme will be prominent in this course, with mentored small-group sessions addressing issues in professional identity formation, wellness and resilience, career discernment, and preparation for residency.
-
Block 9: Transition to Clerkship
The goal of the Transition to Clerkship (2 Weeks) course is to provide an overview of the clinical rotations, along with the knowledge, skills and attitudes required to be successful in the clinical clerkships and electives. This course also sets the stage for the longitudinal Phase 2/3 clinical connections and competencies (C3) course of the Illinois Medicine Curriculum.
Clinical clerkships and electives focuses on experiential learning where students are a part of the healthcare team providing patient care. Given the complexities of the healthcare systems, students will be expected to participate in various educational modules that provides an introduction to the various topics such as credentialing, patient safety, occupational exposure. Students will also have the opportunity as a part of the immersion experience, to observe the management of patients in an inpatient hospital settings. As a part of the immersion experience, the students will obtain a complete history and perform a physical exam in a hospitalized patient and receive feedback on their data gathering and clinical problem solving skills from upper classmen or residents. This opportunity will help ease the transition into the first clinical clerkship experience.
Program directors expect their incoming interns to be prepared to take of patients effectively and efficiently day 1 of residency. Entrustable Professional Activities (EPAs) is a framework that will be used to guide the development of skills and competencies of the learners and ensure that students are ready to perform certain functions without direct supervision on the first day of residency. Students will be introduced to these EPAs and also provided an overview of how they will continue to build their skills over the course of Phase 2 and 3.
-
Doctoring and Clinical Skills (DoCS)
Doctoring and Clinical Skills (Longitudinal) is the primary vehicle for the Clinical Practice theme and students’ introduction to the care of patients. The course will combine classroom exercises and discussion in small groups, skills practice with patient-instructors and with each other, clinical simulation-based exercises for instruction and assessment, in-hospital practice of the complete history and physical examination, and office-based primary care experience in working with patients.
-
Medical Colloquia
Medical Colloquia (Longitudinal) Given the extraordinary amount of curricular content addressed in the typical pre-clinical MD curriculum, and necessary to prepare students for Step 1 of the USMLE examination, course syllabi are usually limited to addressing these high priority issues and are very tightly scheduled and controlled. Yet issues related to medicine are a vital part of everyday news, and bear some relationship to nearly every other academic discipline at the university. The Medical Colloquia offer a varied menu of lectures, seminars, and brief presentations by faculty, students, and guest speakers from Chicago and around the world. The format can be used to augment other courses’ content with presentations on medically-related events in the news, introduce students to the perspectives of other health professions, and provide a venue for topics in the Health, Illness & Society, Health Care Systems, and Professional Development themes that do not fit easily into the schedules of other courses.
For campus specific information, please visit our campus sites: Heading link
View Educational Policies
College-Wide Block Leaders Heading link
| Course | Block Leader(s) |
|---|---|
| Block 1 | Mike LaFontaine, PhD |
| Block 2 | Paul Chastain, PhD and Mahesh Patel, MD |
| Block 3 | Emily Klopp, PhD and Thembi Conner-Garcia, MD |
| Block 4 | Hugh Clements-Jewery, PhD |
| Block 5 | Jenna Regan, PhD |
| Block 6 | Neelofer Shafi, MD and Tracy Soltesz, PhD |
| Block 7 | Monzurul Roni , PhD |
| Block 8 | Jenna Schulte, MD |
| Block 9: Transition to Clerkships (TTC) | Michelle Barnes, MD |
| Doctoring and Clinical Skills (DoCS) | Ani Gangopadhyaya, MD |
| Medical Colloquia | Christina Wells, MD |